Sara Gottesman, M.D., is passionate about skills teaching. From training amateur boxers to equipping Habitat for Humanity volunteers with homebuilding techniques, she has been shaped by the opportunity to master skills, assess what and how she learned, and share these lessons with others.
Now, as a third-year internal medicine resident, Gottesman continues to pursue this passion for instruction — only this time, she’s assisting her peer physicians in training while elevating patient care standards, all while working to save lives in the process.

Sara Gottesman, M.D.
Through her Distinctions in Care Transformation project, a component of Dell Med’s signature Advancing Care Transformation curriculum for residents, Gottesman is increasing access to a frequently-needed procedure while helping internal medicine residents master the execution of the procedure with ease and confidence.
Q&A With Gottesman:
What is diagnostic paracentesis? What are you doing to improve how trainees learn the procedure?
Patients with serious liver disease often build up fluid in their abdomen. This fluid can become infected, which can make the patient very sick or even kill them. A diagnostic paracentesis is a procedure where we use a small needle to sample and test the built-up abdominal fluid for bacteria and white blood cells, which helps us confirm infection and select the right antibiotic to treat the patient.
The original diagnostic kits are large and include extra pieces for procedures other than diagnostic paracenteses, which makes it difficult for trainees still getting comfortable with the procedure. I created a simplified diagnostic paracentesis kit with only the necessary supplies along with clarified instructions to address this. The idea was to make a kit that was easy for the residents to access, fast to use and reduce any confusion or discomfort that may come with using the more complicated kit currently available to us.
Instead of the original kit’s complicated needle and multistep catheter system, the new kit has an angiocath — a small needle with an integrated catheter. These are more commonly used to start IVs, but they are easy to direct and have a part of the device where fluid will “flash,” allowing residents to confirm they are pulling fluid from the right area.
I’m most proud of the instructional sheet that I made to go with the kit: It’s an illustration that reminds residents how to set up for the procedure, how to perform the needle tap to retrieve fluid and how to order the appropriate labs after the sample is collected.
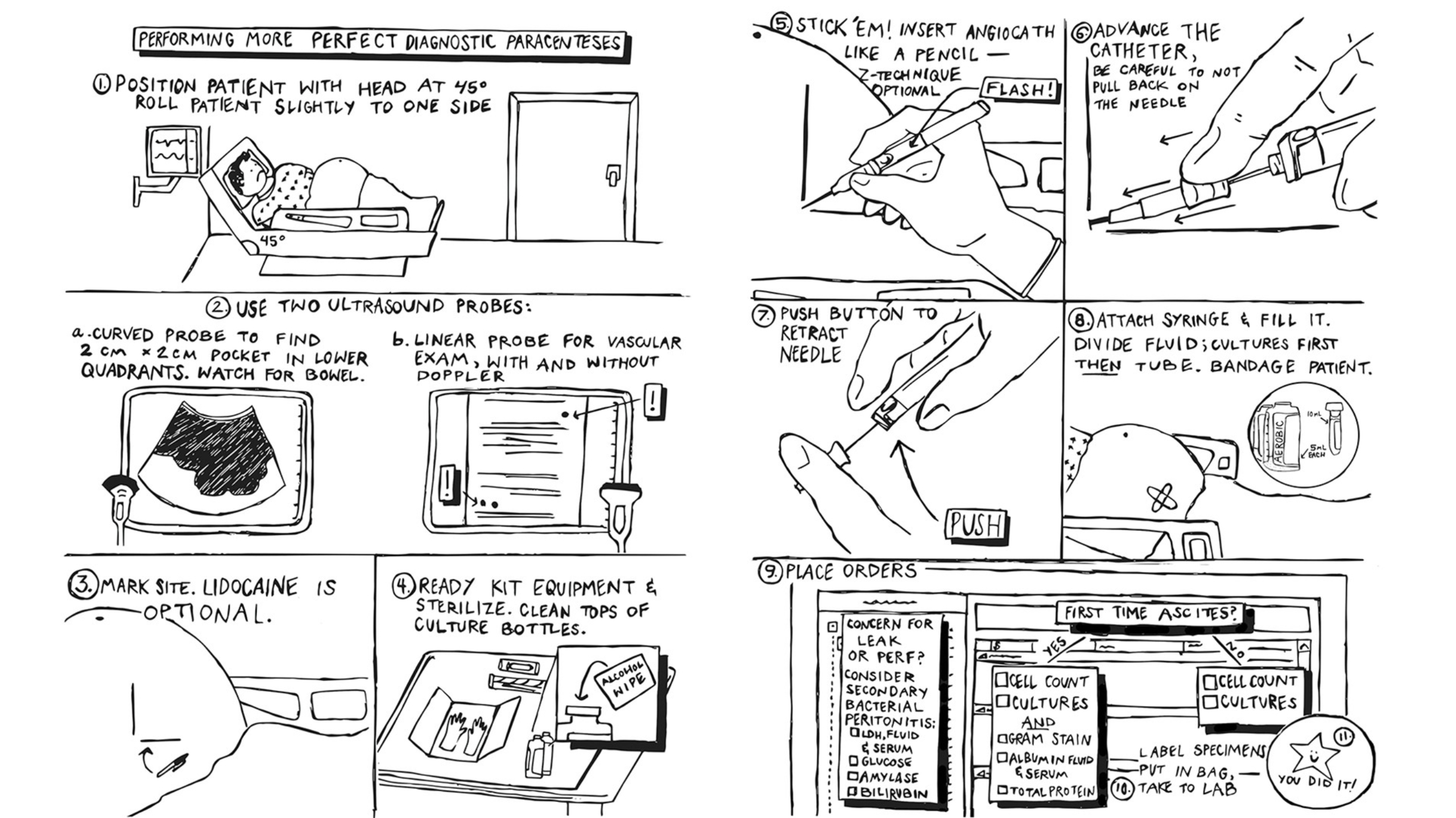
Gottesman’s illustration aids residents in setting up for diagnostic paracentesis, providing instruction on how to perform a needle tap to retrieve fluid and how to order the appropriate labs after the sample is collected.
I personally struggled to understand written or video instructions available in other resources and wanted to develop something more approachable to diffuse some of the anxiety around doing the procedure. The new kits live in the resident workrooms, so they are easier to find than the original kits that are only available in certain supply rooms. So far, many of the residents have used the kit and report that they feel more confident doing diagnostic paracenteses. It is my hope that I can find a way to have the project continue on after I graduate to guide future trainees through diagnostic paracentesis, ultimately expanding patient access to the procedure.
Is there a moment or memory that has influenced your passion for this work?
I think back to when I was a new resident intern and was struggling to adjust. I called a resident from the University of Louisville who was my upper-level resident when I was a medical student and asked her for advice on how to be a good intern. She told me how to organize my thoughts to become more efficient in the parts of my job that were taking me more time, and assured me that my difficulties in adjusting to intern year were normal and encouraged me to stick with it.
Now I make sure to remind my medical students and interns that they can call me in the future if they ever need help, no matter how long it has been since we worked together. My upper-level resident’s guidance made all the difference to my success in my own intern year — I hope that I can pay it forward.
If readers remember one thing about you or your work, what do you hope that is?
I hope that readers take away the idea that making people feel comfortable, even in ways that might seem silly like a cartoon illustration for medical residents, can go a long way in addressing long-standing problems and ultimately enhance patient care.
Graduate medical education, or GME, refers to the period of education in a particular specialty or subspecialty following completion of medical school. This continuation of training through residency and fellowship programs provides the clinical and educational experience needed for physicians to achieve autonomy, deliver high-quality patient care, and prepare for challenges in an evolving health care landscape.
Dell Med serves as the academic home and Ascension Seton as the clinical home for nearly 500 resident and fellow physicians within 50 residency and fellowship programs ranging from family medicine and neurology to pediatric emergency medicine and cardiovascular disease.